“Older people live well, age well and have a respectful end of life in age-friendly communities”
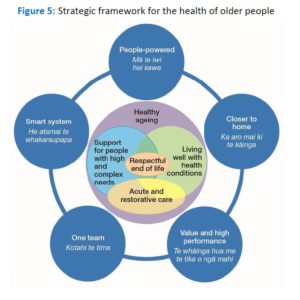 This is the vision set out in the draft of the update of the Health of Older People Strategy that is being finalised by the Ministry of Health. The final Strategy is expected to be released towards the end of 2016.
This is the vision set out in the draft of the update of the Health of Older People Strategy that is being finalised by the Ministry of Health. The final Strategy is expected to be released towards the end of 2016.
Overall the draft Strategy reads well and sets out a good and positive vision for health of older people. The Action Plan included in the draft Strategy showed how the much of a challenge it is to translate the vision into meaningful actions to impact on older people’s wellbeing, with some areas pretty light on commitments for actions in the next two years.
How the progress of the Strategy is measured, reported, evaluated and how it can be designed to be truly responsive to the changing times is also crucial. We are looking for clear signals from Government about the priority of the Strategy, and how the measured outcomes used in the Strategy are linked to Government Better Public Service and other Health Targets.
Wellbeing of the older person at the centre
The term “wellbeing” is used a lot in the draft Strategy. It is difficult to assess whether the wellbeing of older people has improved or not since the current Health of Older People Strategy was introduced in 2002.
In 2014 international expert Dr Satya Brink looked at the question “Is New Zealand a good place to age?” Her work showed that in many respects New Zealand is a good place to age in comparison to other wealthy, developed countries. She did however flag clear areas of concern around income levels for older people very vulnerable to changes in superannuation policy, and the high rate of obesity among older people. Housing is also a real issue with the declining rate of home ownership, especially for Māori, and a lack of data about the supply of accessible housing.
It will be important to include meaningful and internationally comparative measures of progress in improving wellbeing into the strategy, such as the United Nations Madrid indicators.
Social Investment – Crucial Role of Non-government organisations
It is the work of agencies based in communities with networks of volunteer and wider community support that make up a vital part of the web of support that enables people to live well for longer in their home and community and reduces or delays the need for higher level health services. NZCCSS recently released the Valuing Lives, Living Well report that documents some of the ways non-profit, faith-based organisations within our membership networks add value and wellbeing in our communities. The Health Strategy’s focus “social investment” in health will need to recognise the organisational specific capital and the wider social value contributed through community based organisations in making decisions about funding services. If it does not, the Strategy is unlikely to succeed in maintaining or improving health and wellbeing for older people.
Equity and reducing inequality
The draft Strategy has numerous references to equity issues and the need to focus on vulnerable and high-needs population groups. The generation that has been strongly impacted by increasing income and wealth inequality of the past 30 years is ageing and the health and social system must respond well and address the underlying social and economic causes of inequality, especially poor housing quality and inadequate household incomes. It will take genuine cross-government commitment to actions to reduce inequalities that in turn reduce the need for higher level health services in the medium to long term.
Treaty relationship
The draft Strategy states “we recognise and respect special relationship with the Crown through the principles of the Treaty of Waitangi” (p.5), guided by the He Korowai Oranga, the Māori Health Strategy. It recognises that older Māori are among those most impacted by inequities in health outcomes and the need to achieve health equity for Māori.
The Action Plan does include some specific actions in relation to health of older Māori under health promotion, health workforce development, culturally appropriate home and community support service models, flexible commissioning of services to meet the needs of specific population groups including older Māori. The underlying challenge will be for the strategy to fully incorporate responsive ways to involve Māori in measuring better outcomes and reduced inequity into the strategy reporting and evaluation process.
Action Plan
The Action Plan is the place where the vision of the Strategy is made real. The actions identified for the first two years of implementation show the challenge this presents. Current commitments are allocated under the categories of the Strategy and it is hard to tell where specific new initiatives are to be found. Implementing the Strategy will require more focus on the social aspects of health such as the cultural, spiritual, whānau and family needs and less on the “medical model of health”.
Healthy Ageing
Healthy Ageing includes a strong focus on age-friendly communities, which it can only be hoped will mean a similar commitment to better resource this work that is currently left up to the willingness of mainly local authorities to engage and fund this work. A comparatively modest upfront investment in developing more age-friendly communities is likely to bring strong health and social benefits in the medium to long term.
The actions in this area also identify the need for better coordination of services and NZCCSS points to the role of navigators to help people access the services available and the role of day programmes in helping people to stay healthy in their communities. A greater range of housing also has an important role to play in reducing isolation especially encouraging more flexible housing options and requiring wider use of universal design principles in new housing.
Acute and Restorative Care
Integration of acute care services is a theme of the actions proposed. Despite much talk of service integration over many years, there is a feeling that not enough progress has been made and there is a need to prioritise further development of services that genuinely link primary, secondary, community-based and residential aged care services in a way that works for older people and their families. The Ministry of Health should seek endorsement to take the lead in cross-government work on service integration, to help overcome the difficulties of driving work across different government departments.
Living Well with Long-term Conditions
NZCCSS looks for effective actions and leadership from the Ministry of Health to significantly improve the conditions and pay levels for those working the sector. The quality and effectiveness of the paid carer workforce along with better support for unpaid family/whanau carers will be decisive in influencing how well older people are able to continue to live well with long-term conditions in the community.
The challenge that the increasing impact of dementia poses for the health of older people is covered in detail in the Strategy. But the current Dementia Framework actions do not equate to a comprehensive national dementia strategy and plan. Other areas of mental illness need priority as well and NZCCSS also asks if obesity among older people is receiving enough attention.
Support for People with High and Complex Needs
The aim of integrating funding and services around the needs and aspirations of older people is good and offers an opportunity to explore different ways of working and commissioning services. The Strategy seems to be looking at taking the Whānau Ora commissioning approach into wider context, which is one alternative approach to purchasing services. The report of the Productivity Commission inquiry into social services in 2015 set out a range of approaches to commissioning health and social services and an effective Strategy will need to take account of these.
Day programmes play a vital role in improving social interaction for vulnerable older people living in the community as well as providing respite for their family carers but receive little attention in the Action Plan. NZCCSS’ own survey of members in 2015 confirmed the importance of these programmes for the older people attending as well as their carers. The provision and funding of such programmes varies greatly around the country and their contribution to the HOP Strategy goals to support people to live well in the community needs more recognition.
Respectful End of Life
The both the home based support and aged residential care sectors are closely involved in supporting older people through to the end of life. The debate about how to improve support of older people and their whānau needs to more actively include these sectors. The of Review of Adult Palliative Services completed this year has not adequately engaged with and taken account of the role of the aged care sector in end of life care. Further work is needed on the distinctive role of home based and aged residential care in end of life care.
Implementation, measurement and review
The draft Strategy and Action Plan have recognised the need to develop a proper measurement and reporting framework as well as the need to involve older people themselves in this process. The trend in recent years seems to be have been one of winding back consumer participation in DHB decision-making processes and a reduction democratic accountability of DHBs. So increasing the involvement of older people themselves will need a focused plan to support culture change in the way the heath system works.
Measuring outcomes and reporting on them will need to include genuine measures of changes in health and wellbeing at national and regional level that are reported against regularly. But this will need to be done in a way that is balanced with a commitment to reducing the administrative barriers, such as contracts requiring excessive documentation and reporting that is neither relevant nor actually used by the funders, as well as and poorly managed tendering and contract processes.
Read the full NZCCSS submission on the draft Health of Older People Strategy:[wpfilebase tag=file id=6561 tpl=’nzccss_pub_file’ /]
